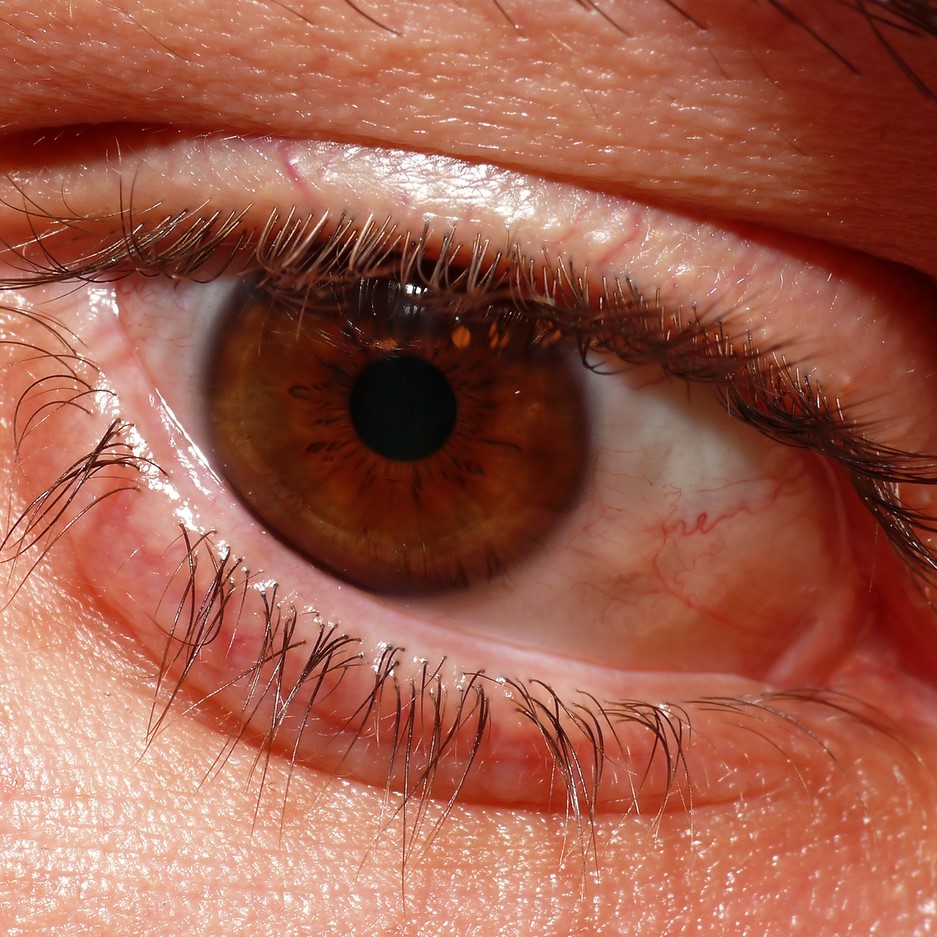
Staining is carried out by instilling 1 drop of 2% fluorescein into the inferior fornix of the affected eye. Fluorescein 2% drops are a useful examination tool, and are stocked in some GP practices. If there is concern that the vision is reduced in the context of a red eye then urgent referral to ophthalmology should occur. Visual assessment is helpful, although this may not be possible in the primary care setting in pre-school children. 1 Reduced vision in a child can lead to rapid decompensation of a squint. 2 The absence of a history of trauma does not exclude injury, as children may be unwilling to disclose an event that may get them into trouble. A history of trauma may be helpful, but it may be difficult to establish the mechanism of injury, thus increasing the chances of a delay in diagnosis. A recent history of viral illness, discharge, and discomfort point towards a diagnosis of conjunctivitis, although significant pain and photophobia are unusual in this setting. Paediatric history taking can be challenging, and in some circumstances the examination findings may yield more useful information than the history. Postoperatively, the vision gradually improved to 6/18 with glasses wear to correct astigmatism, and patching of the right eye to treat amblyopia.īox 2. An examination under anaesthetic was performed and a subtarsal foreign body was found and removed. The superior cornea had localised green fluorescein staining, indicating an epithelial defect in a location frequently associated with a subtarsal foreign body ( Figure 1). Further observation revealed a poor red reflex with scarring of the cornea. On examination he was found to have a vision of 6/60 in the affected eye, blepharospasm (difficulty opening the eyelids), photophobia, pain, ptosis, and lid swelling. He was seen in ophthalmology outpatients 3 months after the onset of symptoms.

While awaiting his eye appointment he continued to be reviewed in primary care, although the presenting condition remained largely unchanged. He was difficult to examine and so was managed initially with chloramphenicol drops and referred routinely to ophthalmology. A 4-year-old boy presented to primary care with a sticky red left eye, new-onset squint, and possible abnormal red reflex.
